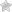Typically found in children, only less than 10% of the people with diabetes suffer from Type I Diabetes [5]. This condition occurs in individuals, where the body is not able to produce enough insulin. Insulin is a hormone which is produced by beta cells of the islet of Langerhans situated on top of the pancreas. Insulin is used by the body to regulate the amount of sugar that is absorbed by the cells of the body. A lack of adequate amounts of insulin in the body lead to an excess concentration of sugar or glucose in the blood stream and it is the primary cause of Type I Diabetes. The condition is believed to be a cause of the immune system of the body destroying the islet cells in the pancreas [4]. Despite all the amount of active research being conducted, there is still no complete cure for Type I Diabetes and managing the symptoms with treatment is the only option available to sufferers.
Juvenile Diabetes
Since Type I Diabetes is usually found in children and young adults, it was earlier known as Juvenile Diabetes. It also goes by the name insulin dependent diabetes.
Type I Diabetes is classified as an autoimmune disorder and this is also the primary distinction from Type II Diabetes. The process of auto antibody testing can be used to verify if a particular case of diabetes is a Type I case or a Type II case.
While Type I Diabetes is typically observed in younger people, it can affect people at any age, though the chances of encountering Type II diabetes are far more likely with an individual aging.

Causes of Type I Diabetes
While the exact causes of Type I Diabetes are unknown, it is believed that in this condition, the immune system of the body of a sufferer destroys the insulin-producing beta cells of the pancreas. The result of this process leads to a complete deficiency of insulin in the blood stream.
- HLA or Human Leukocyte Antigens also play an important role in determining the chances of occurrence of diabetes in an individual since these cells help in recognizing the body’s own cells as foreign cells leading to their auto-destruction.
- The pancreas normally regulates the amount of insulin production based on the changing blood sugar levels but in diabetes, insulin is absent to control blood sugar levels. Thus high blood sugar levels may prevail.
- Heredity also has a major role to play in Type I Diabetes, as it is passed on from one generation to other through genes.
- People who are genetically susceptible to diabetes may become diabetic when triggered by environmental factors like diet, viruses, and toxins
- Sometimes, other factors like cystic fibrosis may destroy beta cells that may lead to diabetes resembling type I diabetes and this is called secondary diabetes.
There are some known risk factors which increase the chance of an individual contracting Type I Diabetes. These include:
- A history of the disease having occurred in the family
- The presence of certain genes in the body
- The disease is more prone to affect younger individuals
- People living away from the equator are also believed to be at a higher risk of developing the condition, especially people in Sardinia, Finland and other neighboring regions.
- Other possible risk factors to the disease include an early exposure of infants to cow’s milk, a low level of Vitamin D in the body, exposure to some specific pathogens and virus, consumption of water rich in nitrates, either early or late introduction of Gluten in an infant’s diet and the risk of contracting the disease is also much higher in babies who are born with jaundice.
Signs and Symptoms of Type I Diabetes
Due to deficient insulin production, glucose is not moved into the cells and glucose accumulates in the blood instead of going into cells, the body’s cells are not able to get energy for many important bodily functions and may cause the following:
- Increased urination even more noticeable at night
- Increased thirst due to excessive urination
- Increased hunger because of insufficient energy production.
- Blurring of vision excess sugar accumulation in the lens of eyes suck extra water into your eye. This leads to change in the shape of the lens and blurs the vision.
- Fatigue and weakness as the body isn’t using the calories is not getting the required amount of energy.
- Damage to the body: High blood glucose levels may damage the small blood vessels and nerves of the kidneys, eyes, and heart leading to atherosclerosis, or hardening of the arteries that can further lead to heart attack and stroke. There is a greater risk to becoming more susceptible to various infections, skin ulceration and gangrene in limbs due to poor blood circulation. This may also result in the need for amputation of limbs.
- The accumulation of glucose in the blood may lead to increase in urination as a measure to remove excess glucose. This may result in loss of a big quantity of water, causing dehydration.
- Diabetic ketoacidosis. Without insulin, the body cells become starved of energy for which the body has to break down fat cells producing acidic chemicals called ketones as end products to be used for energy. Increased levels of ketones in the blood, causes an increased acidity. This phenomenon of excess sugars along with dehydration and acid accumulation is known as diabetic ketoacidosis that can be life-threatening if not immediately treated.
- Weight loss. Due to loss of sugar in the urine, loss of energy providing calories takes place. This loss of energy along with dehydration contributes to weight loss.
- Symptoms of depression are also very common in sufferers of Type I Diabetes.
If left untreated, Type I Diabetes can also present some serious complications. These may include:
- Diseases of the blood vessels and the heart
- Damage caused to the nerves or neuropathy
- Damage caused to the kidneys or nephropathy
- Damage caused to the foot and the limbs
- Conditions of the mouth and the skin
- Complications related to pregnancies
- Infection in the urinary tract
- Sexual dysfunction in both males and females.
Treatment of Type I Diabetes
Type 1 diabetes is treated with exercise, diabetic diet and insulin. Treatment with insulin includes use of synthetic insulin or insulin analogues that are classified as:
- Rapid acting insulin analogue: Insulin Lispro, Insulin Aspart and Insulin Glulisine are some common rapid acting insulin analogues that are administered within 5-10 minutes of food intake and have rapid but short term effect.
- Long acting insulin analogue: Insulin Glargin and Insulin Determir are long acting insulin analogues that do not have any peak action period and lasts for long once the drug is administered inside the body.
- Other intermediate options: There are a number of other medications which may be prescribed for sufferers of Type I Diabetes such as
- Pramlintide or Symlin injections which helps slow down the digestion of food and in turn limits the release of sugar into the blood stream.
- Medications for high blood pressure which can help prevent the kidneys from damage.
- Cholesterol reducing medications, also known as statins, which can help keep the levels of bad cholesterol and fatty acids in check.
- Aspirin and other drugs which can prove to help protect the heart from damage.
There are also many investigational treatment methods available for Type I Diabetes, which are increasingly growing in popularity [1] [3]. While these methods have not yet been conclusively adopted by people, they may prove to be of great help in treatment of some specific cases. Such investigational treatment methods include:
- A transplant of the pancreas: While such a transplant surgery can be potentially risky and not all surgeries are successful, a transplant of the pancreas can allow individuals to successfully lead a normal life without requiring constant insulin medication. This method is usually only used in severe cases of Type I diabetes or when the sufferer requires a kidney transplant as well.
- Transplantation of the islet cells: This is a relatively new method which is being actively researched. While this method has had to face a number of problems in the past, newer drugs and better medical techniques have greatly improved this method. In this method, the available healthy islet cells are protected from the immune system of the body and are also encouraged to expand.
- Transplant of the stem cells: There is active research being done in stem cell research. In studies and clinical trials, it has been demonstrated that patients suffering from Type I Diabetes could refrain from using insulin and lead a healthy and normal life for up to five years after the transplant. While this technique can seem to be appealing, stem cell transplant is still in its nascence and it is a risky procedure.
- Research is also being carried out in order to create a vaccine containing the auto antigen, GAD65. Sufferers who had received this vaccine demonstrated an increased protection of the beta cells. However, this method is not fully approved yet and clinical trials are being conducted in the US and in Europe.

If you suspect that you are at a risk of Type I Diabetes, you need to get a screening and an evaluation done at the earliest. On diagnosis of the disease, proper medical attention will need to be provided with a complete healthcare team consisting of a certified educator on diabetes, a dietician, a social worker, an ophthalmologist or eye specialist and a podiatrist or a foot specialist.
You will also need to understand all of the risks and the complications that Type I Diabetes has to offer. Since the disease has no definite cure, sufferers must ensure that they keep complications in check and manage the symptoms as best as possible.
References
[1] Diabetes Treatment — Bridging the Divide, Kristina I. Rother, M.D.; 356(15): 1499–1501 – Apr 12, 2007 – DOI: 10.1056/NEJMp078030, http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4152979/
[2] The past, present, and future of genetic associations in type 1 diabetes, The Barbara Davis Center for Childhood Diabetes, University of Colorado Denver, Aurora, CO 80045-6511, USA; 11(5):445-53 – October 2011 – DOI: 10.1007/s11892-011-0212-0, http://www.ncbi.nlm.nih.gov/pubmed/21792535?dopt=Abstract
[3] Type 1 diabetes: etiology, immunology, and therapeutic strategies, van Belle TL, Coppieters KT, von Herrath MG; 91(1):79-118 – Jan 2011 – DOI: 0.1152/physrev.00003.2010, http://www.ncbi.nlm.nih.gov/pubmed/21248163?dopt=Abstract
[4] Virus infections in type 1 diabetes, Coppieters KT, Boettler T, von Herrath M; 2(1):a007682 – Jan 2012 – DOI: 10.1101/cshperspect.a007682, http://www.ncbi.nlm.nih.gov/pubmed/22315719
[5] Type 1 diabetes: recent developments, Devasenan Devendra; 2004;328:750 – March 25, 2004 – DOI: 10.1136/bmj.328.7442.750, http://www.bmj.com/content/328/7442/750?variant=full